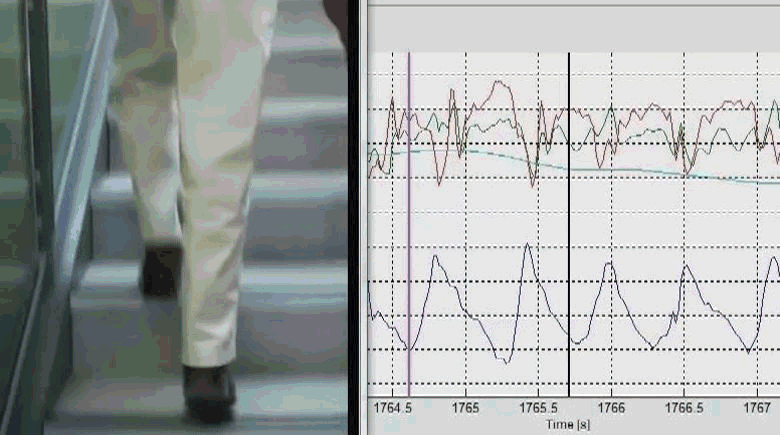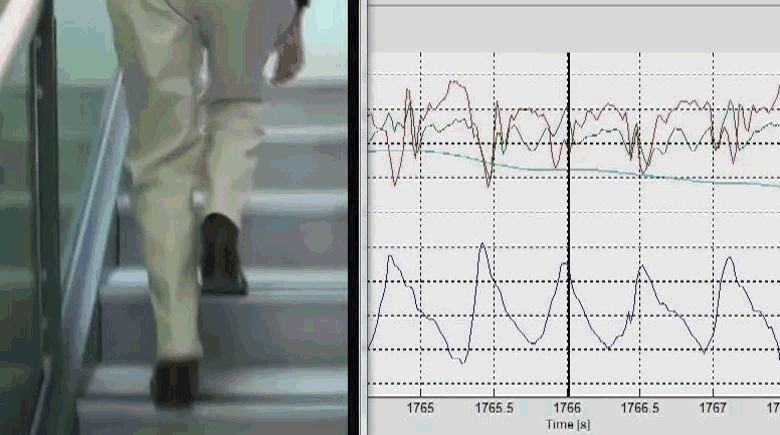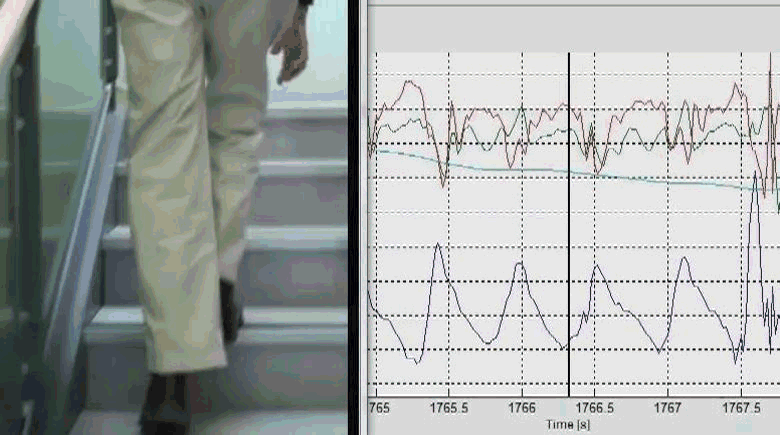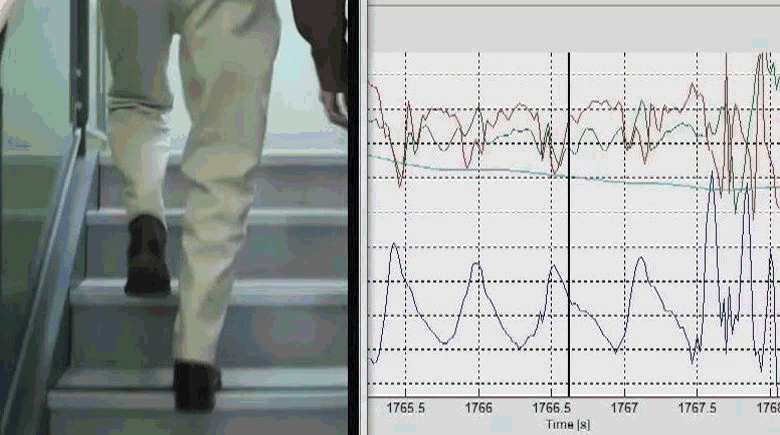
We investigated whether a freely worn pendant inertial sensor, containing a triaxial accelerometer and a barometer, could be used to accurately identify stair ascent by 52 older adults in free living. Stair ascent could be identified using a decision tree, by scaling the barometer threshold to the rate of pressure change to accommodate both athletic and frail older adults with different cadences. 4-fold grid search optimisation was used to determine the decision tree thresholds and achieved Kappa 0.92 with accuracy 99.8%. Sensor-derived measures of stair ascent performance, comprising descriptors of intensity, variability and stability, were compared with prospective falls as well as a battery of clinical fall risk assessments using Spearman’s rank correlations. In our healthy older people, fall related outcomes appeared more related to mental rather than physiological and health factors. Cautious double stepping strategy could be identified remotely. Stair ascent performance was correlated with ascent strategy (r = -0.67), age (r = -0.44), concern about falling (r = -0.43), fall risk scores (r = -0.41), processing speed (r = -0.38), and contrast sensitivity (r = 0.32). Follow-up falls were correlated with ascent stability (r = -0.35). We concluded that pendant-based remote analysis of stair ascents is feasible and may be useful in monitoring of daily activity. The ascent strategies we observed in some people may have reflected an appropriate behavioral response to increased concerns about falling. With increasing acceptance of wearable devices in health applications, reduced functional performance and altered strategies for undertaking activities of daily living could be routinely tracked to augment health care monitoring.