Over the past two decades there has been a steady trend towards the development of realistic models of cardiac conduction with increasing levels of detail. However, making models more realistic complicates their personalization and use in clinical practice due to limited availability of tissue and cellular scale data. One such limitation is obtaining information about myocardial fiber organization in the clinical setting. In this study, we investigated a chimeric model of the left atrium utilizing clinically derived patient-specific atrial geometry and a realistic, yet foreign for a given patient fiber organization. For this purpose, we used an ex-vivo Diffusion Tensor Magnetic Resonance Imaging (DT-MRI) fiber database, which to date is the best available resource for real patient fiber data.
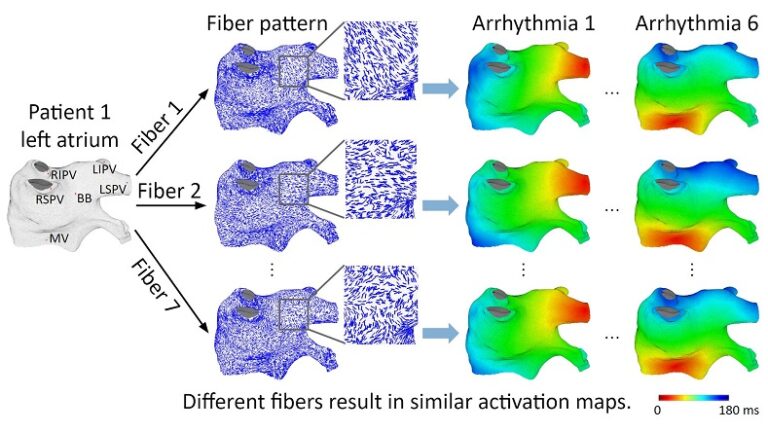
On one left atrium, we conducted 42 experiments: 6 focal arrhythmias each with 7 fibers. We discovered that despite significant variations, the individual fiber organization had a relatively small effect on the macroscopic spatio-temporal activation pattern, independent of the location of the arrhythmia source. Our study showed that low sensitivity of the macroscopic activation pattern to the underlying fiber organization, “the cancellation effect”, is the result of significant differences in the epicardial and endocardial fiber orientations, as well as significant variations in fiber orientation within the epicardial and endocardial layers. Fiber organization can affect activation patterns locally, however, these local effects cancel each other out at the macroscopic level, resulting in similar overall activation patterns.
These findings may have important practical implications leading to significant simplification of patient-specific modeling of atrial arrhythmias by utilizing fiber-independent models.