Ventricular tachycardia (VT) is a life-threatening arrhythmia. In patients with myocardial infarction, electrical activation of the ventricles is impaired by the remodelling of the infarcted area, which results in conduction blocks, and slow conducting zones with sparse surviving fibres. Slow conduction may allow the activation wavefront to travel with a delay larger than the refractory period of healthy myocytes, allowing healthy myocardium to be excited again, thus forming a re-entrant VT circuit.
Catheter interventions consist of identifying such circuits and breaking them by radiofrequency ablation. When a sustained VT occurs, intra-cardiac electrical catheter recordings allow propagation delays to be measured. Thus a 3D activation map of the VT circuit can be reconstructed. Ablation then consists of applying radiofrequency heating across the critical zone of slow conduction, at the core of the VT circuit, acting as a barrier to prevent reentry. However in most cases, VT is not well tolerated by the patient and the lengthy activation mapping cannot be performed. Additionally, after the identified circuit is ablated, in some cases a secondary circuit occurs (during the procedure or after several months).
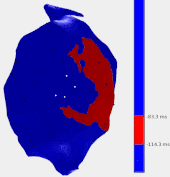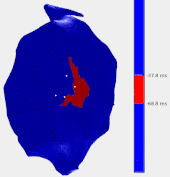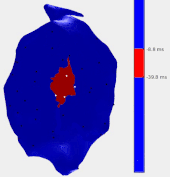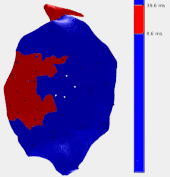
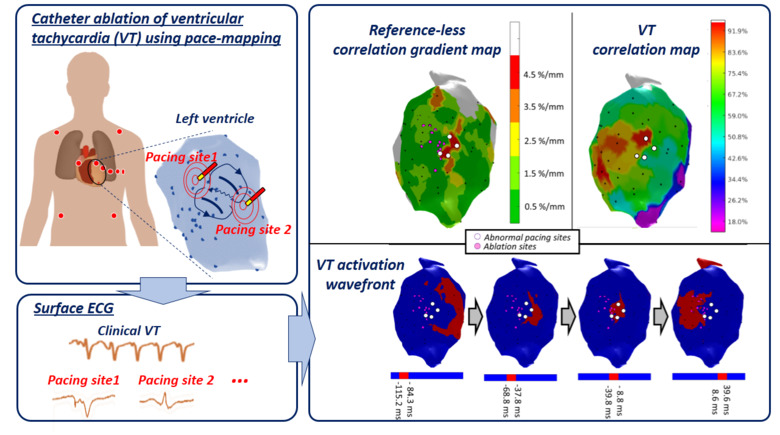
In this work an alternative is proposed, based on the pace-mapping technique. Pace-mapping consists of stimulating the heart with the catheter from different sites of the ventricular cavity, in order to produce activation pathways originating from each of these sites. As the catheter is moved, changes of the activation pathway can be observed by analyzing changes in the surface electrocardiograms (ECG). Areas of abrupt changes are hypothesized to correspond to the critical zones likely to sustain VT circuits. To validate this hypothesis, data from 24 VT ablation procedures were retrospectively analysed with the proposed pace-mapping method (termed “reference-less” as it does not need any reference ECG recording of the VT) and compared to conventional methods for identifying ablation targets.