The last century has seen a gradual increase in global average temperatures—a phenomenon that has come to be known as global warming. The World Meteorological Organization (WMO) has reported that 2020 was one of the three warmest years on record and that the global average temperature was ~1.2 oC above preindustrial (1850–1900) levels [1]. Adverse effects on health resulting from global warming are important issues to consider, as health risks associated with such extreme heat are anticipated [2]. In fact, this warming has been shown to severely limit human activity in tropical and mid-latitude regions [3], and in particular, outdoor and manual workers who are exposed to ambient heat during working hours are susceptible to increased health risks. Thus, workers should pay attention to their own physical conditions and proactively keep out of the heat to rest when uncomfortable. Additionally, supervisors must manage worker’s physical conditions and schedule regular breaks. Therefore, in this trial a new integrated system was developed to notify individuals at risk based on their thermal physiology. This method uses biological and environmental information obtained directly via wearable sensors and the estimated body core temperature collected on-ground cannot be measured wirelessly and noninvasively [4].
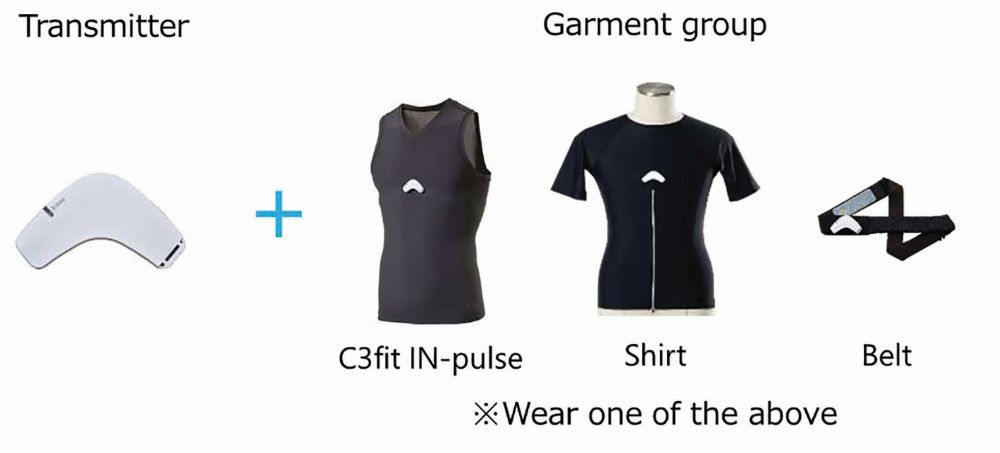
Wearable biological and environmental sensors
It is essential to acquire various biological and environmental information without interfering with work to estimate the risk of poor physical conditions posed to each worker in real-time. Wearable sensors have provided a promising means for such purposes.
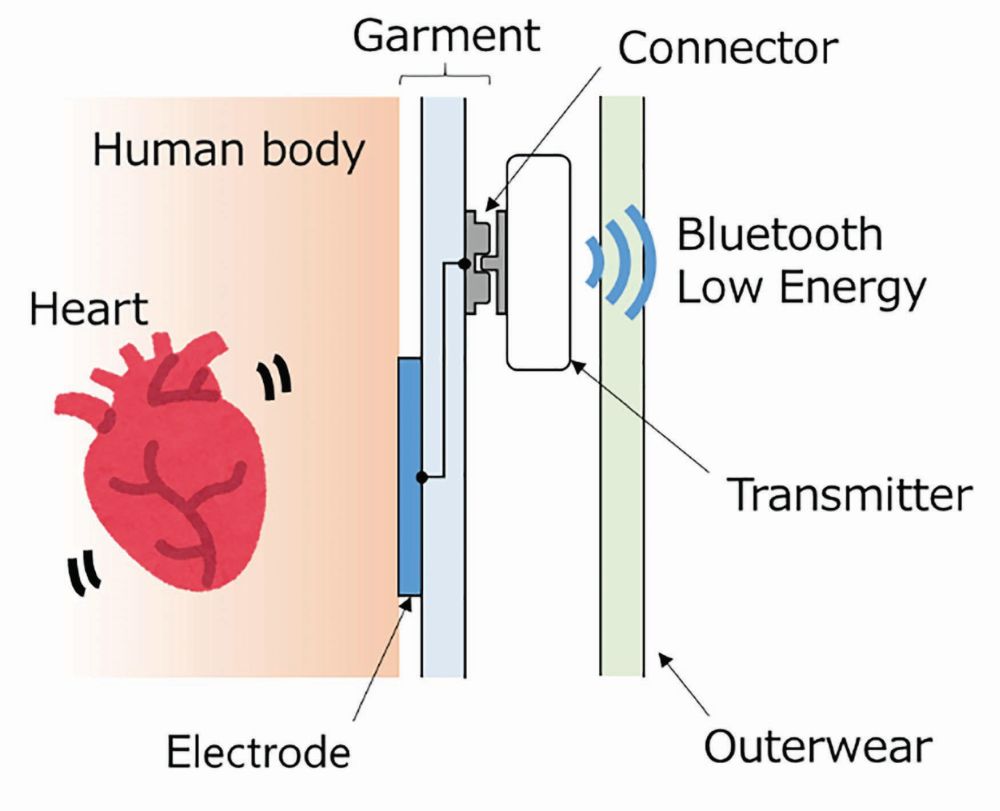
Figure 1 shows the developed wearable biological and environmental sensors [5]. It consists of a transmitter (TX02) developed at the NTT Device Innovation Center, a Hitoe shirt/Hitoe belt from Toray Industries, Inc., or the C3fit IN-pulse from Goldwin Inc.; Hitoe is a performance fabric developed using nanofiber technology. It is gentle on the skin while being worn for extended periods. Figure 2 shows a schematic of the data acquisition process. The user wears the garment as underwear such that the Hitoe electrode, made of conductive textile, is in direct contact with the skin and links the transmitter to the garment via the connector. The electrocardiogram is acquired by the electrode, input to the transmitter via the connector, and recorded as electrocardiographic data. In addition to the bioelectric signal sensor, the transmitter has a built-in temperature/humidity sensor and acceleration/angular velocity sensor. Thus, it can measure electrocardiographic, temperature, and humidity data inside the clothes, in addition to the acceleration and angular velocity of the upper body.
Estimation of core temperature variation
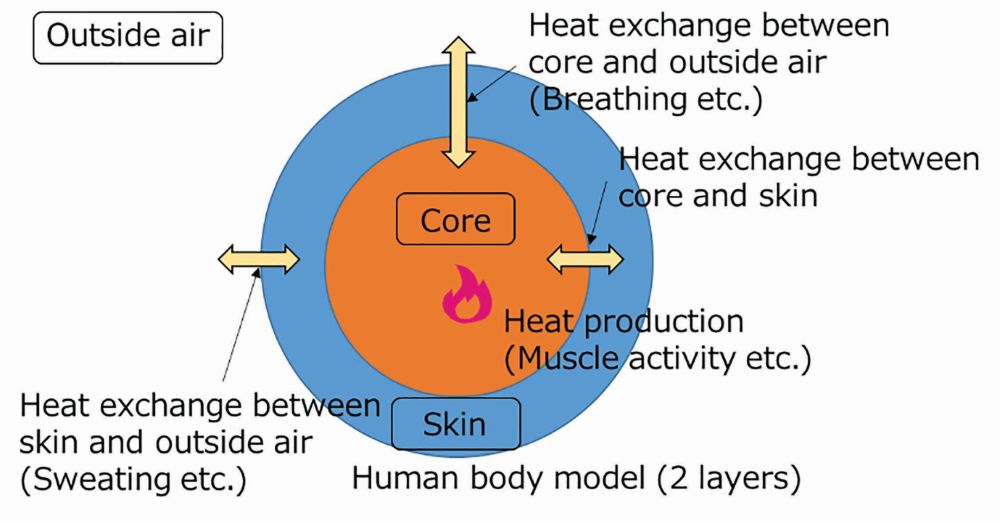
The core body temperature, heart rate, and subjective symptoms of dizziness and nausea are listed as indicators of the risk of poor physical conditions in hot environments [6]. Consequently, we established a new method to estimate the core temperature variation in real-time while performing an activity [7]. In this method, the body temperature variation is estimated by processing the information acquired from the wearable sensor using a newly developed calculation model. An outline of the calculation model is shown in Figure 3. In this model, the human body is divided into a core and skin layer, and the heat exchange between each layer and the outside air is formulated. The formula uses an algorithm that considers factors such as heat produced by human activities, thermoregulatory function due to sweating, and clothing. Heart rate, temperature/humidity inside clothes, and personal information (age, height, weight, gender, and clothes, among others) are input to this model to calculate the variation in core temperature. The model is designed to be simple yet effective, as the computation needs to be performed using limited computation resources (smartphones) in real time.
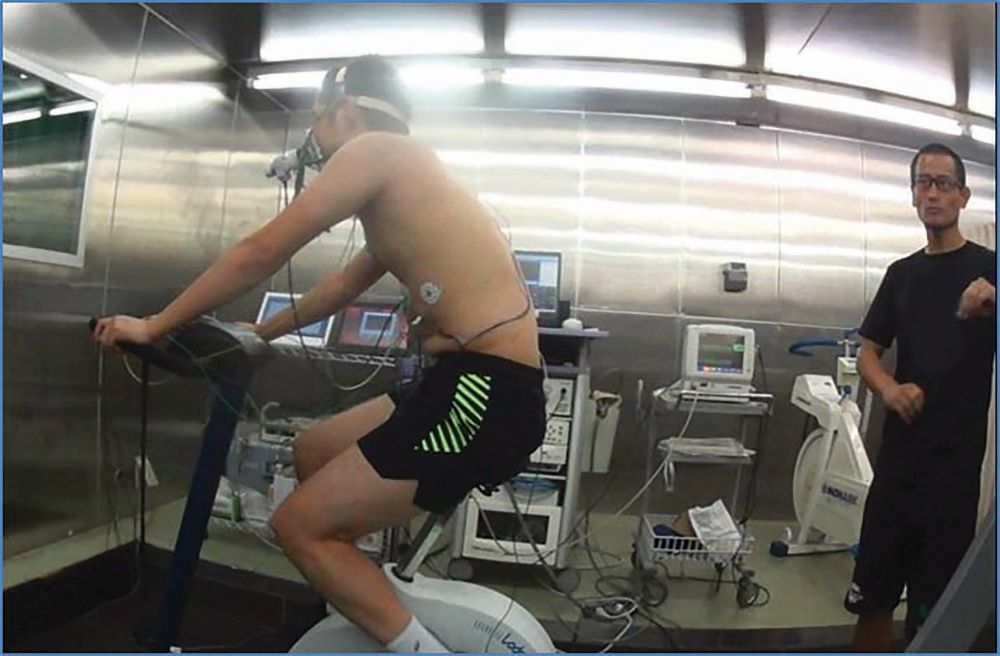
To verify the efficacy of this technique, we conducted a clinical experiment, in an artificial weather room at Shigakkan University to simultaneously estimate body temperature variations using this model. We captured measurements via a rectal thermometer, as shown in Figure 4. The estimation accuracy was confirmed to be 0.15 oC [8].
Criteria and algorithms are required to determine the high risk of poor physical condition for each worker. We set criteria for three indicators: heart rate, estimated core temperature fluctuation, and subjective information based on joint experiments and thermal physiology. We also developed an algorithm that determines the overall risk of poor physical conditions, determined via the state of the three indicators, and issues an alert in the case of high risk.
Application to construction team at the world’s largest sports event in 2021
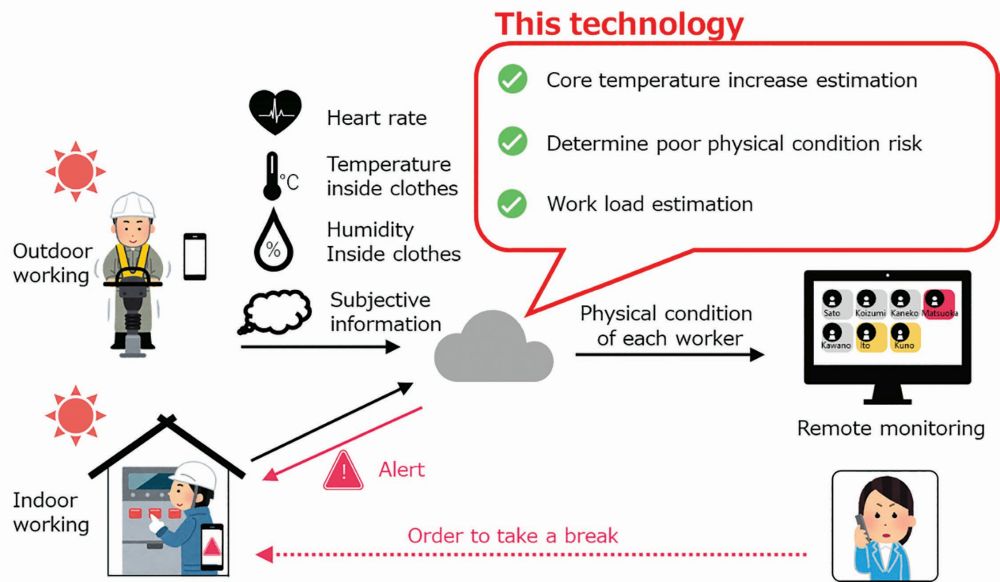
Figure 5 shows a schematic diagram of our health risk alert system applied to 49 construction workers employed during the summer of 2020 at the world’s largest sports events to be held in Tokyo (total number of 834 person-days from August 5 to September 30). We implemented the core temperature variation estimation technology, the poor physical condition risk determination technology, and the workload estimation technology into a smartphone app as a health risk alert tool for occupational safety. We also built a system that remotely monitors the physical condition of each worker wearing the wearable biological or environmental sensors via the cloud. Alerts were sent to workers who were identified as being at high risk. Risk cases were comprehensively detected during the construction period by supplementing each case with the three indicators of poor physical condition risk determination technology (heart rate, core temperature increase, and subjective information). Alerts were sent to remote monitoring systems, workers, and supervisors. Workers receiving the alert paid attention to their own physical conditions and proactively kept out of the heat to rest before uncomfortable. Simultaneously, according to the alerts their supervisors assessed workers’ physical conditions and directed a break. Since no serious cases of poor physical condition such as heat stroke occurred during the construction, we consider that this health risk alert system is useful.
Health management of workers and volunteers, who are essential for the event operation, is one of the crucial topics in addition to the safety of athletes. Nippon Telegraph and Telephone East Corporation made plans to apply this health risk alert system to the construction and maintenance workers for the world biggest sports events held in Tokyo, summer 2021. Future studies may include the application of the system to athletes as well as different individuals, including other outdoor and manual workers, such as firefighters and outdoor police officers.
References
- World Meteorological Organization, “Climate change indicators and impacts worsened in 2020,” Press Release 19042021, Apr. 19, 2021. [Online]. Available: https://public.wmo.int/en/media/press-release/climate-change-indicators-and-impacts-worsened-2020
- International Labor Organization, Working on a Warmer Planet: The Effect of Heat Stress on Productivity and Decent Work, Geneva, ILO, 2019.
- J. P. Dunne, R. J. Stouffer, and J. G. John, “Reductions in labor capacity from heat stress under climate warming,” Nature Climate Change, vol. 3, pp. 563–566, 2013.
- L. Wong, “Temperature of a healthy human (body temperature),” in The Physics Factbook, Aug. 22, 2007. [Online]. Available: https://hypertextbook.com/facts/1997/LenaWong.shtml
- K. Kuwabara, A. Tokura, Y. Hashimoto, Y. Higuchi, and H. Togo, “Wearable biological/environmental sensor and its application for smart healthcare services,” NTT Tech. Rev., vol. 18, no. 10, pp. 46–51, Oct. 2020.
- ACGIH: Threshold Limit Values and Biological Exposure Indices, 2019.
- A. Hirata et al., “Estimation of core temperature form heart rate and ambient conditions using two-layer two-component model,” IEEE Access, submitted for publication.
- K. Takagahara et al., “Physical condition management technology for making a more comfortable work site,” NTT Tech. Rev., vol. 19, no. 6, pp. 48–54, Jun. 2021.



