Cardiovascular diseases are the leading cause of mortality worldwide. Central arterial pulse wave velocity (PWV) is a marker of arterial stiffness and an independent predictor of cardiovascular disease and incident hypertension. Moreover, PWV is pressure-dependent, wherefore surrogates like pulse arrival time (PAT), i.e., the time interval elapsing between the ECG R-peak and a peripheral waveform pulse, have been widely investigated for cuff-less blood pressure (BP) estimation. However, PAT is typically biased by 1) an unknown cardiac delay and 2) inhomogeneous mechanical properties of the peripheral vasculature.
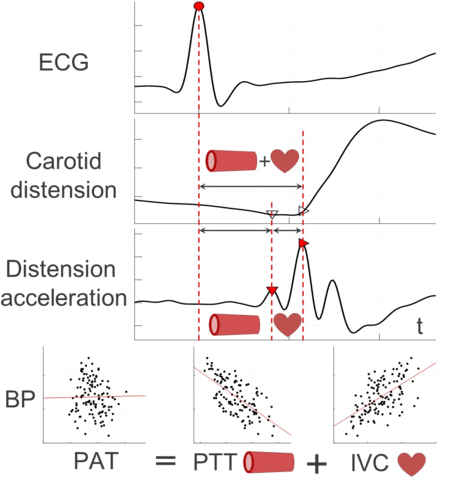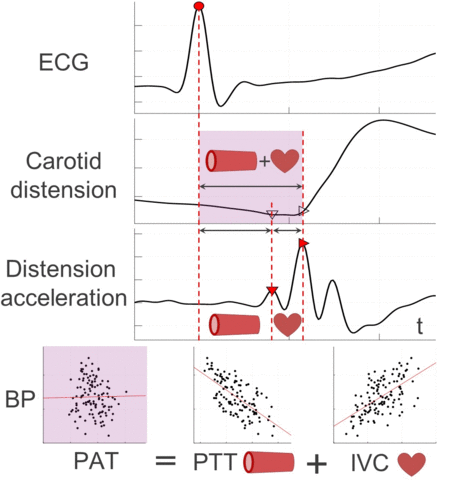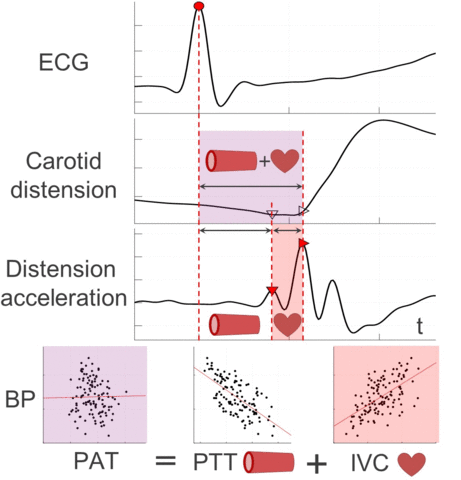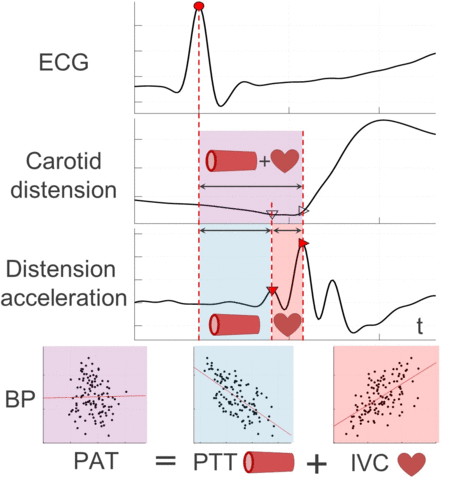
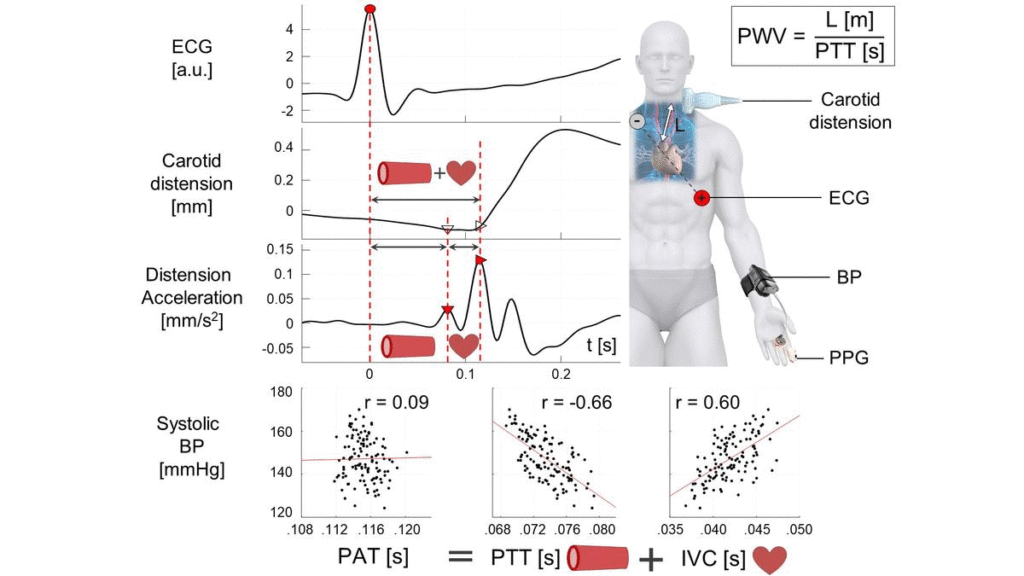
Therefore, this work presents a novel ultrasound-based method for central PAT segmentation into cardiac isovolumic contraction (IVC) and vascular pulse transit time (PTT) intervals. More specifically, these subintervals are segmented at a manifestation of the IVC onset in the carotid artery distension waveform, which is caused by a minor pressure perturbation from mechanical cardiac-aortic coupling and signaled by a characteristic fiducial point preceding the systolic upstroke.
Data was obtained in a small-scale cohort of 10 human subjects with BP ranging from normotension to stage two hypertension. Carotid artery ultrasound, ECG, noninvasive continuous BP and a finger photoplethysmogram were simultaneously recorded, allowing for the direct comparison between central PTT and conventional peripheral PAT. Accordingly, central and peripheral PWVs were computed from the respective intervals and estimated arterial path lengths (L), and correlations with the established Bramwell-Hill PWV and BP references were analyzed by linear regression.
Compared to peripheral PAT-based PWV, the central PTT-based PWV explained more than twice as much inter-subject variability in Bramwell-Hill PWV. Furthermore, diastolic and systolic BP, estimated from central PWV, undercut the IEEE mean absolute deviation threshold of 5 mmHg, unlike BP estimated from peripheral PWV. Thereby this proof-of-concept study demonstrates a practical method for unilateral assessment of central PWV, bearing the potential to improve cardiovascular risk prediction in clinical routines.