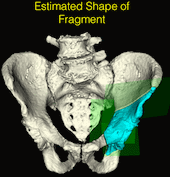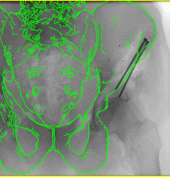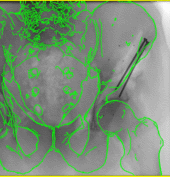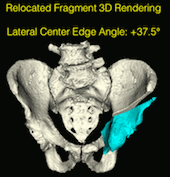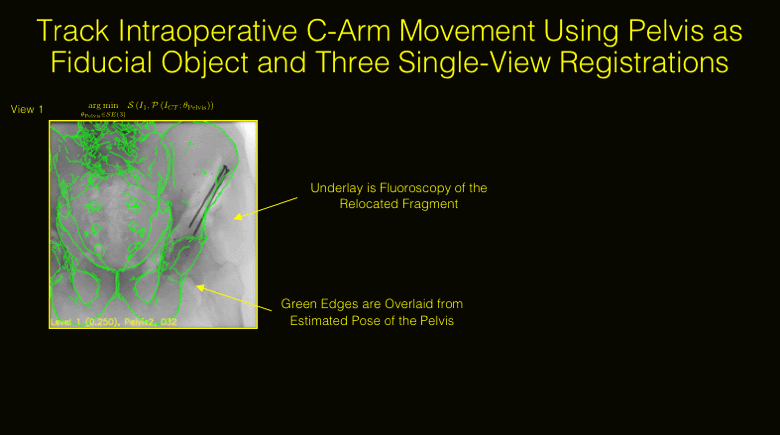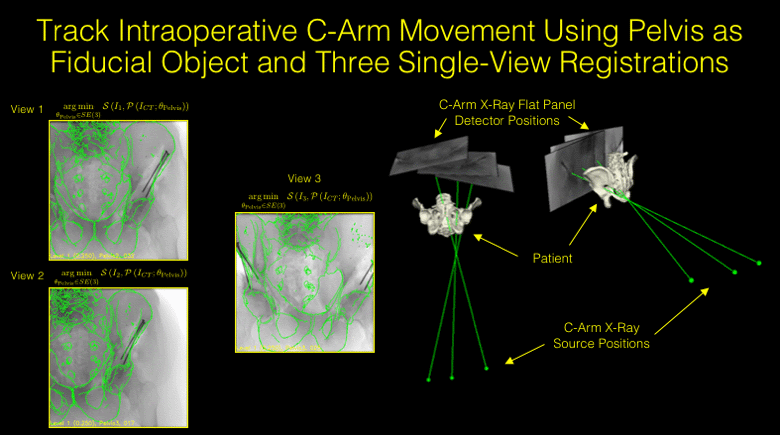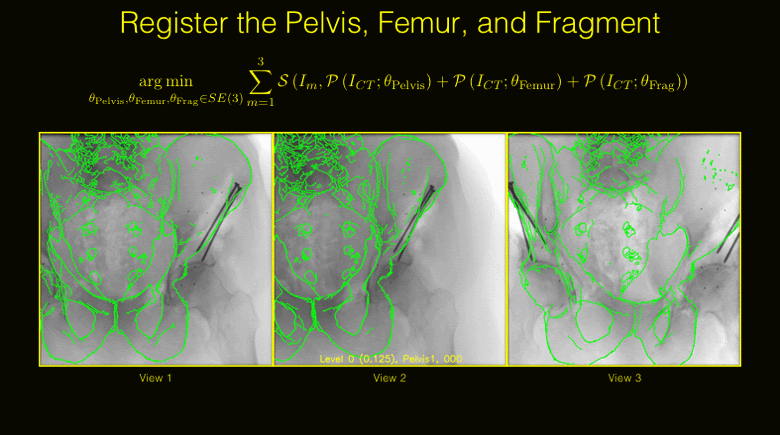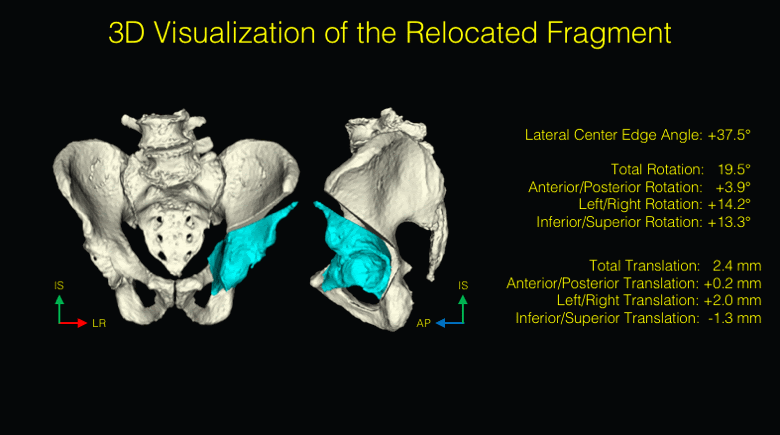
State-of-the-art navigation systems for pelvic osteotomies use optical systems with external fiducials. In this paper, we propose the use of X-ray navigation for pose estimation of periacetabular fragments without external fiducial objects. A multiple-object, multiple-view, two-dimensional/three-dimensional registration pipeline was developed to recover fragment pose. Intraoperative pelvis registrations of the first fluoroscopic view are initialized using an approximate annotation of a single anatomical landmark in the view. Pelvis registrations of subsequent views are automatically initialized using a search about the C-arm’s orbit. Relative poses between all views are recovered using the patient’s pelvis as a fiducial object. Preoperative osteotomy plans are refined to more accurately match the intraoperative shape using osteotomy boundaries in the fluoroscopic images. The pelvis, femur, and updated fragment are registered using all views simultaneously. The pipeline was tested through an extensive simulation study and six cadaveric surgeries. In simulation, average fragment pose errors were 1.3°/1.7 mm when the planned fragment matched the intraoperative fragment, 2.2°/2.1 mm when the plan was not updated to match the true shape, and 1.9°/2.0 mm when the fragment shape was intraoperatively estimated. In cadaver experiments, the average pose errors were 2.2°/2.2 mm, 3.8°/2.5 mm, and 3.5°/2.2 mm when registering with the actual fragment shape, a preoperative plan, and an intraoperatively refined plan, respectively. Average errors of the lateral center edge angle were less than 2° for all fragment shapes in simulation and cadaver experiments. In conclusion, the proposed pipeline is capable of accurately reporting femoral head coverage within a range clinically identified for long-term joint survivability. Human interpretation of fragment pose is challenging and usually restricted to rotation about a single anatomical axis. The proposed pipeline provides an intraoperative estimate of rigid pose with respect to all anatomical axes, is compatible with minimally invasive incisions, and has no dependence on external fiducials.