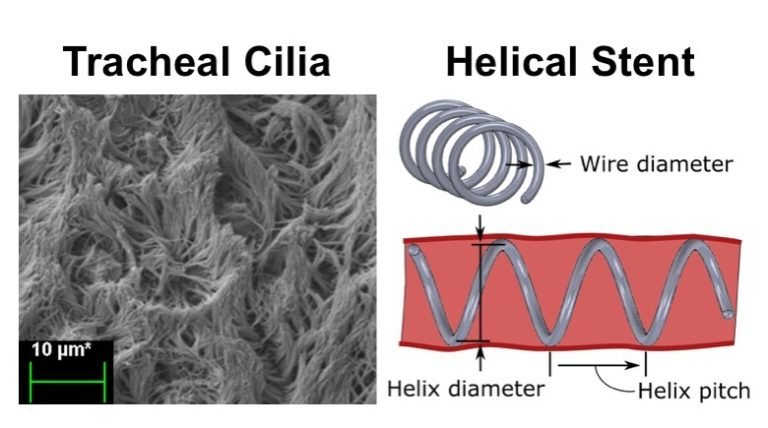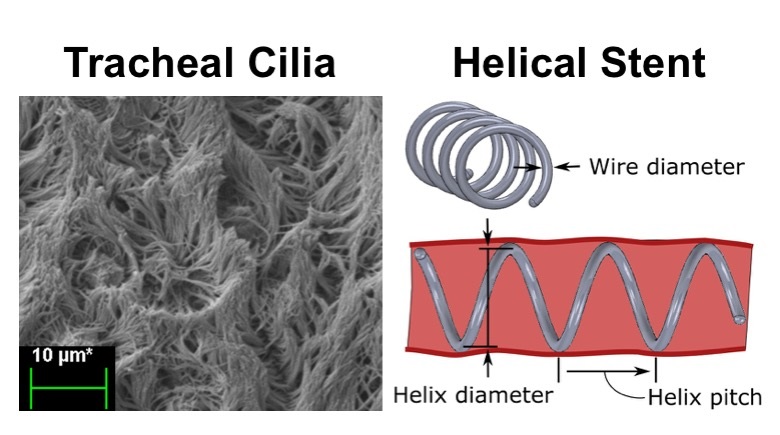
The standard treatment for tracheobronchomalacia in infants and children is to use positive pressure ventilation to prevent airway collapse. With a treatment period of 3-9 months, maintaining a child on a ventilator requires close monitoring to ensure regular mucus clearance of the endotracheal tube. The inability to clear mucus leads to an increased risk of airway infections including pneumonia and tracheitis. The goal of this work was to develop a pediatric airway stent for treating tracheobronchomalacia that could be used as an alternative to positive pressure ventilation. An uncovered helical stent design is described that provides radial airway support without blocking ciliary mucus transport. Its helical shape resists migration while also enabling atraumatic removal despite epithelialization using an extraction technique similar to removing a corkscrew from a cork. Tools for stent placement and removal are also presented. A mechanics model of stent compression is derived for selection of stent design parameters (pitch and wire diameter) that provide the desired amount of tracheal support while introducing the minimal amount of foreign material into the airway. Worst-case airway area reduction with stent support was investigated experimentally using a pressurized tracheal phantom matched to porcine tracheal tissue properties. The stent design was then evaluated through in vivo porcine experiments. Phantom testing validated the mechanics model of stent compression. In vivo testing demonstrated that the stent was well tolerated by the animal. Since the helical design covers only a small portion of the epithelium, mucus transport through the stented region was minimally impeded. Furthermore, the screw-like stent resisted migration while also providing for atraumatic removal through the use of an unscrewing motion during removal. The proposed stent design and tools represent a promising approach to preventing airway collapse in children with tracheobronchomalacia.