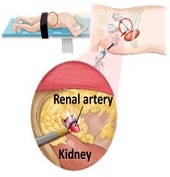
The radical sympathectomy and percutaneous catheter-based renal denervation (RDN) are two techniques proposed to treat life-threatening resistant hypertension. However, sympathectomy has been abandoned due to the procedure being too invasive, and RDN resulted in variation in blood pressure reduction between patients due to suboptimal denervation. Thus, a method to effectively ablate renal nerves while not being very invasive is needed to treat the resistant hypertension patients. Here we propose a minimally invasive Laparoscopic Denervation System (LDS) to serve this unmet clinical need.
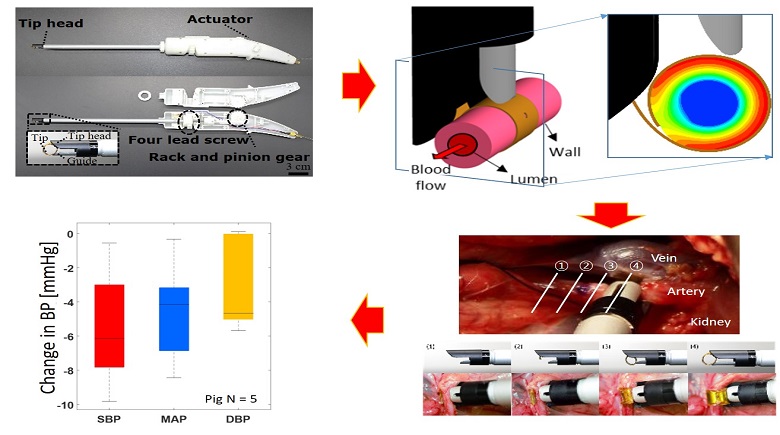
The LDS employs a direct renal nerve ablation technique, where the tip of the flexible surgical instrument softly wraps the renal artery and ablates the renal nerves while not imparting thermal arterial damage. The In-silico simulations and in-vivo swine model study were performed to demonstrate the clinical effectiveness of the LDS. Extensive simulations revealed that the proposed LDS localizes the heat distribution between the electrode and the outer arterial wall, thus denervating nerves without damaging the artery. The acute swine study and histological analysis confirmed the simulation findings and showed that the nerves around the artery were completely denervated, and the artery lumen was intact. The acute systolic blood pressure was reduced by 9.55 mmHg after surgery.
The LDS presented here can ablate the renal nerves safely and effectively, independent of anatomical variation and nerve distribution. LDS’s advantages over catheter-based RDN far outweigh the disadvantage of being slightly more invasive due to laparoscopic in nature. The proposed LDS approach is innovative and inventive and presents a novel technique to treat hypertension in real-world applications. The proposed method can be expanded to other therapeutic modalities, e.g., for treating autonomic nervous system disorder.