A man walks into the Emergency Room at Massachusetts General Hospital (MGH) in Boston, MA. He has just returned from Liberia, where an Ebola epidemic rages. He has a fever, is nauseous and has been vomiting. Quickly assessing the situation, the ER nurse puts the emergency room on lockdown and instructs hospital personnel to don personal protective equipment (PPE), head-to-toe gear resembling a hazmat suit. The patient is moved by wheelchair to a secure isolation room, or buffer zone, to be cleaned and prepared to enter the hospital for treatment. At the same time, other staff members are preparing a critical-care room where the patient will remain for the duration of his stay. Doctors and nurses carry checklists to review protocol measures, and perhaps most importantly for the sake of containment, the removal and disposal of the protective suit once contact is over.
This event never happened with an actual Ebola patient, but the drama did play out in the fictional world, as part of a simulation drill held at Boston’s largest and oldest hospital late last year. It followed on the heels of a similar, and by now notorious, real-life case at a Dallas Hospital in September 2014 that was not handled as well. In the aftermath of that case in which two nurses became infected with the Ebola virus, many people, including the general public and healthcare workers themselves, were asking one critical question: just how prepared are American hospitals—so gleamingly high-tech and proudly well-equipped—to deal with the types of infectious diseases that routinely devastate other parts of the world and which can so easily circle the globe aboard any one of the thousands of flights traversing the planet each day? And when that disease finally does arrive in American hospitals, will those hospitals be as prepared as they imagine themselves to be?
“If you ask most emergency planners or hospital ER staff, most of them believe that a major infectious-disease outbreak will start overseas and give us a lead time to plan for it, and that is certainly not a guarantee,” says Paul Biddinger, Medical Director for Emergency Preparedness at Massachusetts General Hospital. It’s a misconception that’s led to gaps in preparedness and unwise budget cuts at a national level. In the case of Ebola, are we learning from previous mistakes or merely scraping by?
Fighting Infections on a Global Scale
The Centers for Disease Control and Prevention (CDC) has been tracking infectious disease threats globally for more than 60 years with a workforce that includes more than 300 internationally deployed public health professionals plus close to 1330 locally employed workers in nearly 60 countries. The organization works with political leaders to create programs that target reducing the spread of commonly transmitted diseases such as AIDS, influenza, and cholera, and most recently, of course, Ebola.
Last year, as the number of Ebola cases began rising globally, the CDC issued response-planning tips and guidelines for healthcare providers, both at state and local levels, stressing the importance of rapid identification and proper personal protective equipment and offering resources to help state and local jurisdictions address self-identified gaps in Ebola response planning. A statement from the CDC’s spokesperson Jason McDonald explains that the CDC’s Office of Public Health Preparedness and Response (OPHPR), which was established in 2002, leads the agency’s preparedness and response activities by providing strategic direction, support, and coordination for activities across the CDC as well as with “local, state, tribal, national, territorial, and international public health partners.” Furthermore, the CDC provides funding and technical assistance to states to build and strengthen public health capabilities.
According to McDonald, OPHPR receives approximately $1.5 billion in annual funding from Congress to build and strengthen national preparedness for public health emergencies including natural, biological, chemical, radiological, and nuclear incidents. McDonald says Congress appropriates over three-quarters of this funding for two CDC programs, one of which is the Public Health Emergency Preparedness cooperative agreement and the other the Strategic National Stockpile. “As we have said often and have seen recently with Middle East Respiratory Syndrome and Ebola, infectious diseases are only a plane ride away,” says McDonald. “Improving detection and response in other countries can help reduce the threat of a disease outbreak arriving on U.S. shores.” It is for these reasons, McDonald says, that the federal government started its Global Health Security (GHS) initiative.
In February 2014, representatives from 29 nations, the European Union, the World Health Organization, the Food and Agriculture Organization of the United Nations, and the World Health Organization for Animal Health met in Washington, DC, and Geneva, to launch the Global Health Security Agenda, pledging a commitment to significantly advance global health security and help prevent, detect, and rapidly respond to infectious disease threats over the next five years. Together, they established nine objectives related to detection, prevention, and response when it comes to infectious disease threats globally.
“Ensuring global health security is a shared requirement and responsibility, and an undertaking that cannot be done in isolation,” Natalie Brown, USUN Rome Deputy Chief of Mission said in June. “Success depends on cooperation and collaboration among countries and institutions, as well as among stakeholders from diverse sectors.”
Preparedness at Local Levels
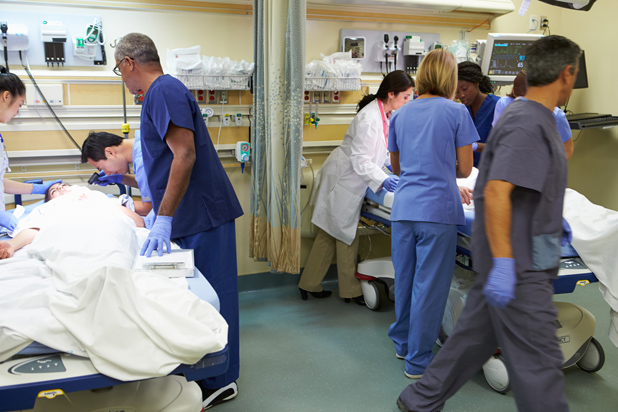
Despite international commitment to infectious disease prep, costly and time-consuming training for unknown future outbreaks is not always a top priority, and it can be difficult for many hospitals to determine what resources they can spare for an epidemic that may or may not come through their doors. “You have to walk that fine line between an event happening and not saying the sky is falling all the time,” Katie Passaretti, head of infection prevention at Carolinas Medical Center in Charlotte, NC, told the Southwest Times Record, an Arkansas daily newspaper, in December. In fact, according to an October 2014 survey by the Association for Professionals in Infection Control and Epidemiology, only about six percent of hospitals claimed they were well prepared for an Ebola patient.
So what does it take to truly be prepared? Variables from one disease to another will always stand somewhat in the way, but experts say it’s about putting the proper systems in place and then practice, practice, practice.
Julia Dunn, Director of the Communicable Disease Control Division at Boston Public Health Commission, says best practices and standard operating procedures inform preparedness in a big way. “Protocol in case of an emergency is actually built on standard operating procedures. Institutions have infection control policies and procedures, and they have training around such policies and procedures. These are practices that are done every day, like wearing gloves and properly handling needles, and they give us a solid base on which to build. Institutions also have policies around employee health. And all this works together in the case of any potential disease outbreak or even a single exposure. It’s about building systems and not waiting for an outbreak. Early identification, engineering controls, personal protection equipment, cleaning, negative airflow: all of this allows for the safe care of people who have a disease that is of significance in terms of public health or communicable disease.”
Dunn is also quick to point out, however, that infectious disease outbreaks are often moving targets so that flexibility within systems is imperative. “Here’s an example,” she says. “For certain populations who are immunocompromised there may be a need for modifications of standard practices. There may be different protocols for these special situations. We need to have systems that are flexible so we can readily modify things. And sometimes there’s the need to change systems as we learn more about an organism or an outbreak we haven’t had a lot of experience with.” Ebola, she says, has required a lot of training around the use of PPE. “Even if you haven’t had a patient you have to prepare this training. There must always be drilling and ongoing training for some of these specialty areas.”
Biddinger is one of the people responsible for drilling and ongoing training in these areas and helped pull together the MGH Ebola simulation mentioned above. In his role at MGH and as Director of the Emergency Preparedness and Response Exercise Program at the Harvard School of Public Health, Biddinger is an active researcher in the field of emergency preparedness and has lectured worldwide on preparedness and disaster medicine. Biddinger says that levels of preparedness will always differ between institutions that practice ongoing training for these situations and those that don’t—and not eveyone can afford the expensive training drills that MGH employs.
“There’s no question that hospitals across the country are at differing levels of readiness for infectious disease threats,” he says. “Some have robust plans that have been tested and that the staff has been broadly educated on and some have less.” One challenge, he says, is that it’s not reasonable—or even possible—to expect that all employees across a healthcare organization know all the details of a bio-threat plan. “We have 25,000 employees [at MGH] and not all of them know the specific details of our Ebola response or other bio-threat response, but they don’t need to,” he says. “Everyone needs to know the basics: How do you ID a suspect case? How do you isolate that case and who do you call for help with further investigation and care? These things everyone has to know.”
In the case of the simulation at MGH, Biddinger says, that the hospital learned some valuable information.
“It was in those tests that we learned some lessons on aspects we wanted to improve but it also gave us great confidence that the base elements of our plan were effective.”
The Trouble with Budget Cuts
Biddinger is quick to point out that drills of this scale are not easy or cheap to carry out—and neither would be treatment in a potential outbreak. “In order to do that exercise we had to empty out two treatment rooms in the emergency department and three in the intensive care unit—some of the most expensive care resources we have.” Approximately 75 people were involved in some way either as supervisors or participants, “So even though it only took a few hours, it represents an enormous commitment of personal space and medical-care resources to go through such a fictional test and make sure we can get it right,” says Biddinger, who estimates that tests of this nature can cost as much as $20,000 each.
In fact, according to the National Association of County and City Health Officials, “the containment, treatment, and contact investigation” of even a small number of Ebola patients has the potential to rapidly overwhelm local health department budgets, as per capita spending on preparedness within the public health sector has decreased by nearly 50 percent in the past year and a general lack of funding has decreased the overall number of preparedness programs nationally.
More than half of local health departments rely solely on the federal government for preparedness funding from the CDC and the U.S. Department of Health and Human Services’ Hospital Preparedness Program (HPP)—both of which have been cut by more than one-third recently.
Experts like Dunn and Biddinger say this poses a problem, for sure. “Funding is a challenge,” says Dunn. “Particularly when we get to areas where ongoing training is necessary. Take Ebola, for example, you need to have people trained to use proper protocol and personal protective equipment, and that kind of training, that kind of drilling, it’s extremely important and yet there’s no funding to support it. Preparedness requires ongoing training and drilling so that when something does happen you’ll be in a better position to respond.”
The Big Picture
Perhaps budget cuts are pointing to a bigger problem—an arrogance within American hospitals that breeds the conception that we’re too advanced to ever really suffer an infectious-disease outbreak of the scale we’re seeing in West Africa. “Are we overconfident in some of our assumptions about the spread of infectious disease?” Biddinger asks. “I think we absolutely are. As we’ve seen with global travel and speed of travel, it’s possible even if [the disease] did start overseas it could arrive here much more rapidly than we’ve previously planned for,” he says. “I think we are also sometimes overconfident in our ability to institute public health infectious-control measures on a wholesale basis and in our ability to get people to behave in a way that we think is most effective for interrupting disease transmission. For instance, how well can we ask people to distance themselves from others? How well can we get them to follow public health guidance and not transmit the disease to others? It’s not certain.”
Dr. Melissa McDiarmid, from the University of Maryland, seems to agree with Biddinger: “If there is any kind of blessing from this Ebola outbreak, it’s that we need to stop making excuses regarding preparedness,” she told the Southwest Times Record in December. And Dunn says while we’re constantly learning from previous health scares, lack of funding works in direct contrast with this notion. “You have to build systems, you have to drill, and train, and evaluate. When we’re not in an outbreak setting, we must continue to work on these systems to strengthen them and enhance their robustness. [Budget cuts and lack of funding] start to erode these processes. Right now investments are being made at some level but I honestly don’t know if it’s enough. Only time will tell.”



