Abstract:
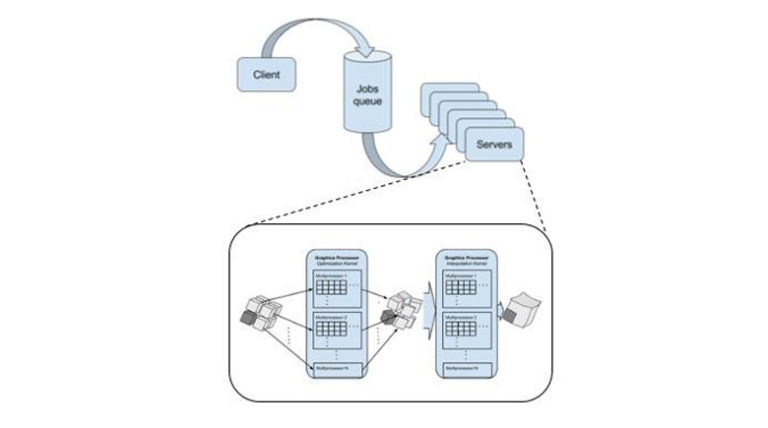
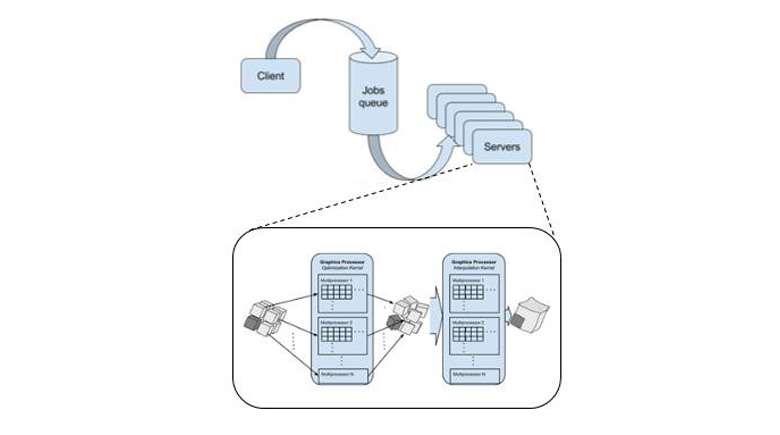
The images generated during radiation oncology treatments provide a valuable resource to conduct analysis for personalized therapy, outcomes prediction, and treatment margin optimization. Deformable image registration (DIR) is an essential tool in analyzing these images. We are enhancing and examining DIR with the contributions of this paper: 1) implementing and investigating a cloud and graphic processing unit (GPU) accelerated DIR solution and 2) assessing the accuracy and flexibility of that solution on planning computed tomography (CT) with cone-beam CT (CBCT). Registering planning CTs and CBCTs aids in monitoring tumors, tracking body changes, and assuring that the treatment is executed as planned. This provides significant information not only on the level of a single patient, but also for an oncology department. However, traditional methods for DIR are usually time-consuming, and manual intervention is sometimes required even for a single registration. In this paper, we present a cloud-based solution in order to increase the data analysis throughput, so that treatment tracking results may be delivered at the time of care. We assess our solution in terms of accuracy and flexibility compared with a commercial tool registering CT with CBCT. The latency of a previously reported mutual information-based DIR algorithm was improved with GPUs for a single registration. This registration consists of rigid registration followed by volume subdivision-based nonrigid registration. In this paper, the throughput of the system was accelerated on the cloud for hundreds of data analysis pairs. Nine clinical cases of head and neck cancer patients were utilized to quantitatively evaluate the accuracy and throughput. Target registration error (TRE) and structural similarity index were utilized as evaluation metrics for registration accuracy. The total computation time consisting of preprocessing the data, running the registration, and analyzing the results was used to evaluate the system throughput. Evaluation showed that the average TRE for GPU-accelerated DIR for each of the nine patients was from 1.99 to 3.39 mm, which is lower than the voxel dimension. The total processing time for 282 pairs on an Amazon Web Services cloud consisting of 20 GPU enabled nodes took less than an hour. Beyond the original registration, the cloud resources also included automatic registration quality checks with minimal impact to timing. Clinical data were utilized in quantitative evaluations, and the results showed that the presented method holds great potential for many high-impact clinical applications in radiation oncology, including adaptive radio therapy, patient outcomes prediction, and treatment margin optimization.