Shokouhmand, Arash; Wen, Haoran; Khan, Samiha; Puma, Joseph; Patel, Amisha; Green, Philip; Ayazi, Farrokh; Tavassolian, Negar
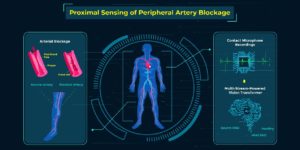
Peripheral artery disease (PAD) is a common condition in which the arteries carrying blood to the legs are narrowed or obstructed. PAD currently affects 8.5 million people in the US, and is either asymptomatic or accompanied by cramping leg pains in early stages. The common clinical test for the identification of PAD is the measurement of ankle/brachial index (ABI), which is defined as the ratio of the systolic blood pressure at the ankle to the systolic blood pressure on the arm. Although the ABI test is a well-established and convenient clinical practice, it offers a low predictive sensitivity of 79%, indicating a considerable rate of undiagnosed PAD cases. Undiagonosed PAD leads to limb soreness, infection, gangrene, and may eventually result in limb amputation. In this study, we introduce and develop an accurate and non-invasive framework for the diagnosis of PAD using abnormal heartbeat patterns caused by the backward flow of blood produced by occluded arteries in the leg. The proposed framework employs a small, sensitive accelerometer contact microphone (ACM) placed on the chest wall to capture abnormal vibrations associated with PAD. A novel neural network coined multi-stream-powered vision transformer (MSPViT) is developed which recognizes abnormal signal patterns associated with PAD emerging in ACM recordings. The input to MSPViT consists of Mel-frequency cepstral coefficients (MFCCs) of 10-second recordings of chest vibrations, coupled with high-level-of-abstraction features obtained from the middle layers of a pre-trained ResNet50 with MFCCs as their inputs. Clinical trials on 74 PAD patients and 32 healthy subjects demonstrate sensitivity scores of 99.45% for PAD detection and 96.66% for severity classification into three groups of healthy, mild, and severe cases. The ACM + MSPViT framework presents a fundamental step towards rapid and accurate diagnosis of PAD, offering a considerable increase in prediction sensitivity compared to the current clinical practice.
Twitter Content:
Researchers at @FollowStevens demonstrate that a contact microphone placed on the chest wall empowered by a multi-stream-powered vision transformer is capable of detecting and classifying the severity of peripherical artery disease (PAD).
Researchers at @FollowStevens develop a novel sensing framework which accurately detects peripheral artery disease (PAD) using abnormal heartbeat patterns caused by the backward flow of blood produced by occluded arteries in the leg.