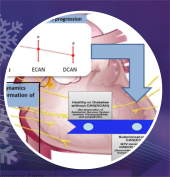
Cardiac autonomic neuropathy (CAN), a major complication of diabetes, is characterized by a gradual increase in damage to the autonomic nerve fibers that results in abnormalities in ventricular repolarization (VR) dynamics. CAN needs to be detected at the subclinical stage, as at the clinical stage positive treatment outcomes are rare. The presence of CAN is difficult to diagnose at the subclinical stage due to the absence of overt symptoms and the widely used cardiovascular autonomic reflex tests (i.e. Ewing test battery) are not sensitive enough for subclinical CAN detection. Therefore, ECG based technique may provide a better alternative to detect CAN at subclinical stage.
In this study, a linear parametric modeling was used to model ventricular repolarization (VR) dynamics from RR, QT and ECG derived respiration (EDR) signals. The study analyzed 80 age-matched participants (40 with no cardiac autonomic neuropathy (NCAN) and 40 with CAN of two different levels). In the CAN group, 25 participants had early/subclinical CAN (ECAN) and 15 participants with definite/clinical CAN (DCAN). The study results showed that QT-RR-EDR model could successfully detect subclinical CAN and describe the gradual alteration of QTV with CAN progression through variation of model fit values whereas QT-RR model cannot. This finding also establishes the importance of adding respiratory information for analyzing the gradual deterioration of normal VR dynamics in pathological conditions such as diabetic CAN.